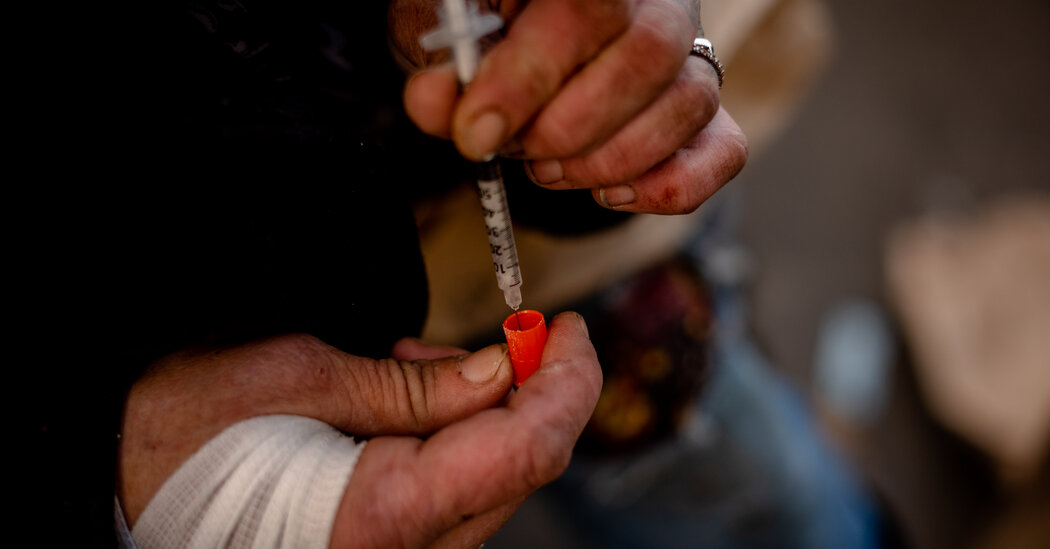
The White House on Wednesday designated a common animal tranquilizer that is increasingly mixed into street fentanyl as an “emerging drug threat,” a formal move that requires the administration to create strategies to enhance law enforcement efforts, health interventions and data collection to combat it.
This is the first time that the White House’s Office of National Drug Control Policy has ever identified a substance for that designation, a mark of the gravity of the danger that it considers to be posed by the drug, xylazine.
Xylazine was approved for veterinary procedures, primarily in cattle and horses, 50 years ago but has never been sanctioned for medical use in humans. Known popularly as tranq or tranq dope, it is a powerful and addictive sedative that slows breathing and heart rate, increases the risk of fatal overdose and often produces severe skin ulcers and abscesses that have led to amputations.
“Many communities are not even aware of the threat in their backyard,” Dr. Rahul Gupta, the head of the drug control office, who is often referred to as the national drug czar, said in a briefing with reporters.
According to a 2018 directive from Congress that established the emerging threat designation, the administration must now lay out plans within 90 days to coordinate a national response to xylazine. That could include creating protocols for treatment, withdrawal and wound care therapies, expanding testing for the drug’s presence and scheduling it as a controlled substance, which would give federal law enforcement agents authority to pursue its illicit use.
Fentanyl Overdoses: What to Know
Dr. Gupta said that xylazine withdrawal could lead to symptoms so intense — such as migraines, double vision and body-rattling anxiety — “that persons may leave medical treatment, including drug treatment, against medical advice.”
But it is sought out by dealers and drug users because it is relatively cheap, with its own addictive properties, whether consumed on its own or mixed with opioids or even amphetamines. Like fentanyl, xylazine first appeared as an adulterant in the illicit drug supply in the Northeast, predominantly in Philadelphia, and then rapidly spread west and south. Citing data compiled by the Drug Enforcement Administration and the Department of Justice, Dr. Gupta noted that in the two-year period from 2020 through 2021, detection of xylazine in forensic labs grew 112 percent in the West and 193 percent in the South.
Currently, the supplies of xylazine are thought to come from China and possibly Mexico, India and Russia, but they could also be coming from some domestic manufacturers who sell to veterinarians.
Wednesday’s announcement follows a crescendo of recent alerts from local health authorities and warnings from other federal agencies. In a xylazine alert in March, the D.E.A. said it had detected the drug in 23 percent of confiscated fentanyl samples in 48 states in 2022. Last November, the Food and Drug Administration, which approved xylazine decades ago for veterinary procedures, issued a nationwide warning to health care providers, and in February, it announced it would monitor imported xylazine for illegal diversion.
Xylazine differs from fentanyl in major ways, which contributed to the administration’s decision to declare it an emerging threat. Unlike fentanyl, heroin or the prescription painkiller oxycodone, xylazine is not an opioid. That means conventional methods for reversing an opioid overdose, like naloxone injections or nasal sprays, may not succeed in fully reviving a person who has used it.
The Opioid Crisis
Xylazine withdrawal symptoms must be managed differently from those of an opioid, and rehabilitation protocols are not yet established. And unlike opioids or, for that matter, amphetamines, xylazine is not listed as a controlled substance, which would make it subject to greater law enforcement scrutiny.
Wednesday’s White House announcement had long been awaited by many community outreach groups and clinics, anxious for direction on how to combat xylazine. Dr. Joseph D’Orazio, chief of medical toxicology and addiction medicine at Temple University Hospital in Philadelphia, which has had perhaps the country’s largest influx of patients afflicted by xylazine, said that research about how the drug works in humans would be critical.
“We still don’t know what causes the wounds, just a lot of conjecture,” he said. “Once that’s understood, maybe we can work up strategies on how to avoid the wounds or treat them better. And we need to understand the withdrawal so we can figure out how to treat it better.”
Dr. Gupta noted that managing xylazine’s licit and illicit uses would be challenging. It is frequently used as a sedative and an analgesic in large-animal medicine, as veterinarians suture wounds, grind down sharpened molars and treated infected hooves. Preserving the drug’s status and access for veterinarians while shutting down supplies to dealers is a topic already under deep discussion.
And Dr. Gupta was candid about the fact that getting a better grip on xylazine, while urgent, would be only a step in long, painful journey. His office is also pressing this effort, he said, in part to look ahead “to what potentially comes after xylazine, as an additive to fentanyl, in order to get in front of the next additive in the drug supply.”